Nursing Home Scheduling: 5 Tips for Improved Staff Efficiency and Resident Satisfaction
Nursing homes face many scheduling challenges that can impact their ability to deliver quality care to residents.
Discover the most common staffing issues in assisted living scheduling, explore ways to overcome assisted living staff shortages, and pick up best practices for effective nursing home scheduling. See the best nursing home scheduling software for long term care facilities.
Discover Agendrix, the smart scheduling solution for long term care facilities. Save time, reduce errors, and improve team communication while ensuring compliance and enhancing resident care. Experience a user-friendly snap schedule scheduling software that adapts to your unique needs. Try Agendrix today and revolutionize your scheduling process!
7 Major Staffing Issues in Nursing Homes
1. Staff Shortages
Many nursing homes struggle with a shortage of qualified nursing staff, including registered nurses (RNs), licensed practical nurses (LPNs), and certified nursing assistants (CNAs). This can be due to a variety of factors such as an aging workforce, low wages, and high turnover rates.
- 96 percent of nursing homes said they are struggling with hiring new staff.
- Almost half of nursing home providers reported that their workforce situation has worsened since May 2022.
2. High Turnover Rates
Nursing homes often experience high staff turnover rates, which can disrupt continuity of care for residents and create an unstable work environment. This can be attributed to factors such as job dissatisfaction, burnout, inadequate training, and insufficient support from management.
- Long-term care facilities lost a total of 307,000 jobs between February 2020 and December 2022.
3. Inadequate Training and Education
Staff may not receive sufficient training and education to effectively care for the diverse needs of nursing home residents, particularly those with complex medical conditions or cognitive impairments. This can lead to a lower quality of care and increased risk of adverse events.
4. Burnout and Stress
Nursing home staff often experience high levels of stress and burnout due to the physical and emotional demands of the job, long hours, and insufficient staffing levels. This can lead to decreased job satisfaction, increased turnover, and a negative impact on the quality of care provided to residents.
5. Compensation and Benefits
Nursing home staff, particularly CNAs, often receive relatively low wages and limited benefits, which can contribute to recruitment and retention challenges. Competitive pay and benefits can help attract and retain qualified staff, ultimately improving the quality of care in nursing homes.
6. Lack of Financial Support
Reimbursement rates for medicaid services in nursing homes are typically lower than the actual costs of care. The Biden Administration is considering implementing a federal staffing minimum for nursing homes to help address these issues. However, a federal mandate without substantial and consistent resources could worsen the situation.
- An AHCA/NCAL report from July 2022 found that nursing homes would have to spend up to $10 billion per year and hire almost 188,000 nurses to comply with increased minimum staffing requirements.
7. Risk of Workplace Harassment
Factors such as high stress, understaffing, and the nature of caregiving work can potentially contribute to an increased risk of harassment. It is essential for management to establish and enforce clear policies for preventing workplace harassment. It also needs to maintain a healthy work environment by addressing any harassment issues promptly and effectively, as well as providing proper training and support to staff.
How to Overcome Assisted Living Staff Shortages
Analyze Your Current Resident Population and Staffing Approach
Determine your resident occupancy and distribution within the facility to see if your staffing strategy is optimized for efficiency.
Make the Most of Your Existing Nursing Home Staff
Nursing home staff is still exhausted by the compassion fatigue, moral distress, and burnout caused by the COVID pandemic. Nursing home managers should schedule skilled staff as optimally as possible. This may entail reviewing all treatment plans, medications, and processes to identify those that can be modified and improved to lighten the burden on staff.
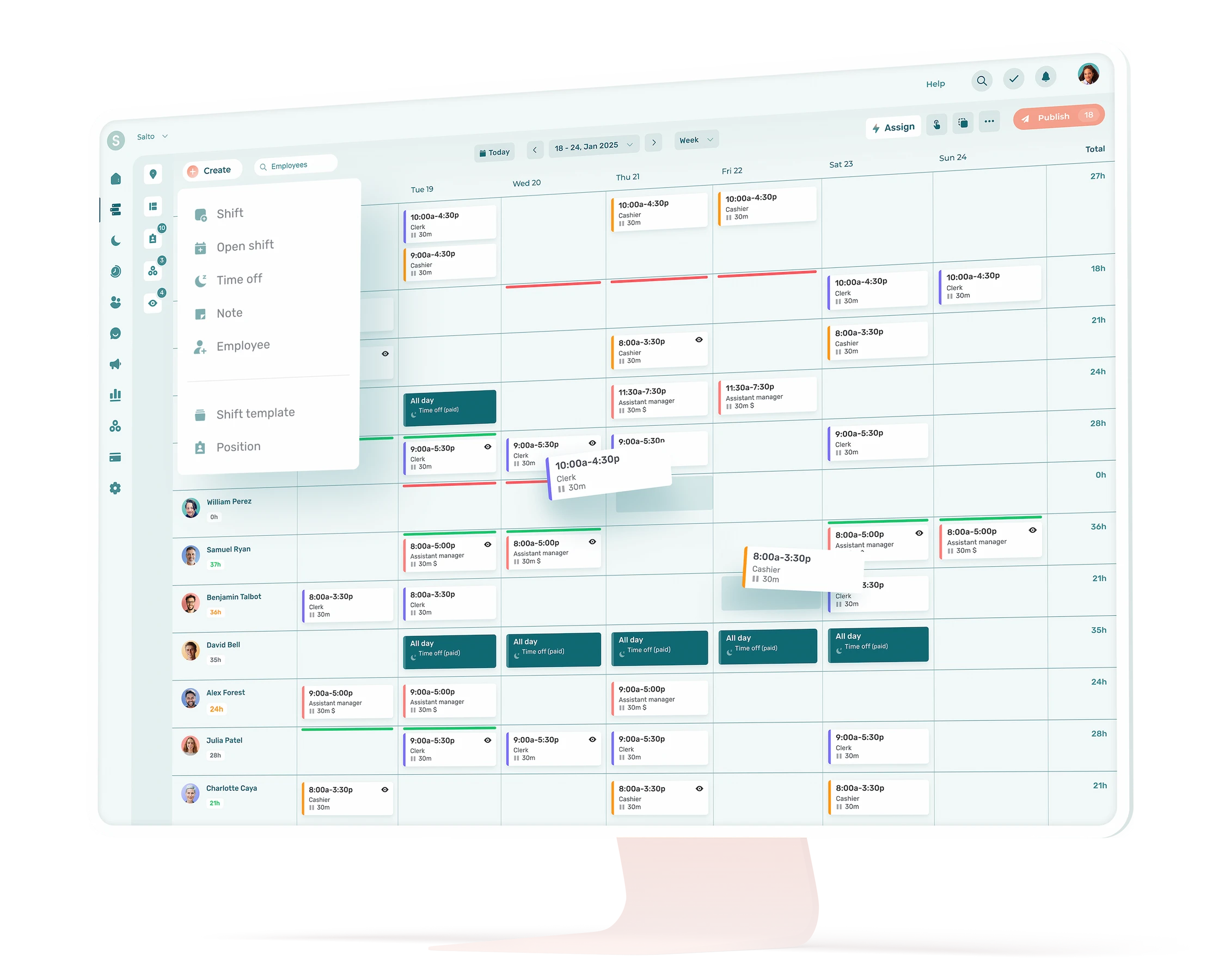
Streamline Scheduling With Technology
Nursing home managers face myriad scheduling challenges, made even worse by the labor shortage. Utilizing timekeeping and staff scheduling software for nursing homes can save hours each week. If you’re struggling with staffing shortages, consider exploring best practices and software solutions to assist administrators in addressing and preventing scheduling issues in your organization.
Allow Flexible Work Schedules
Since the COVID pandemic, the demand and need for flexible work hours has only grown among the working population. It may be time to review your HR policies to ensure they are keeping pace with the changing times. Incorporating flexible scheduling, self-scheduling, and adjustable shift start times may help attract and retain more quality workers.
Categorize Essential and Non-essential Tasks
Nursing home managers should review essential and non-essential tasks, factoring in nursing procedures, care routines, and resident needs. In crisis or triage situations, it’s vital that staff understand this distinction to take appropriate actions.
Utilize Non-nursing Staff
Effective nursing home management strategies involve identifying tasks that non-nursing staff can perform and scheduling them accordingly. For instance, physical therapists and their assistants might assist with transfers, toileting, accident investigations, and fall/injury prevention, easing the workload for other staff members.
Leverage External Staffing Resources
Nursing home managers may not be aware of excellent external staffing resources available. Here are a few options to consider:
- Provider associations, which can offer support and assistance during staffing shortages.
- Your state’s Department of Public Health, which may be authorized to deploy crisis staffing, including National Guard and strike teams.
- Identify and recruit candidates who applied to vaccination clinics but were not accepted due to limited positions.
- Collaborate with home health, hospice, or acute care providers, which can offer valuable resources for alleviating staffing crises.
- Licensed medication assistants and technicians, which can support licensed nurses in states that allow it (check state requirements).
- Your Chamber of Commerce, which can help identify displaced, furloughed, or underemployed individuals who can assist during a staffing crisis.
- The underutilized mature workforce, which might be helpful for filling non-certified support positions.
Review Non-essential Medication Management
Managers can collaborate with physicians and consulting pharmacists to determine if any non-essential medications can be paused during times of worker shortage to reduce staff time demands and increase workflow flexibility.
Do You Need a Nursing Home Scheduler?
Schedulers in nursing facilities play a crucial role in managing staff schedules and ensuring smooth operations. The role has gained importance since the pandemic. It has also become more complex as facilities rely on external staffing agencies and networks.
Although technology like scheduling software can help streamline the shift scheduling process, human input remains vital. Successful schedulers need to be proactive, accommodating, and efficient in managing shift schedules. However, the role is often undervalued, and schedulers are frequently pulled to the floor to work, causing high turnover rates.
Investing in the role and ensuring schedulers have the time and resources to focus on their duties can benefit the overall organization.
5 Best Practices for Effective Nursing Home Scheduling
1. Develop and Maintain a Comprehensive Staffing Plan
Assess the current and future staffing needs of the nursing home based on resident population, acuity levels, and regulatory requirements. Ensure that the staffing plan is regularly reviewed and updated to accommodate changes in the facility’s needs.
2. Provide Flexible Scheduling Options
Offer various scheduling options, such as self-scheduling, part-time and full-time positions. Allowing adjustable shift assignments and start times and letting employees request time off may also meet the needs and preferences of your staff. This can help improve employee satisfaction, retention, and work-life balance.
3. Utilize Scheduling Software and Technology
Use assisted living scheduling software to streamline the process of creating, adjusting, and communicating staff schedules. This can help reduce manual effort, minimize errors, and ensure that staff has instant access to their schedules and any changes in real-time.
4. Prioritize Effective Communication and Collaboration
Maintain open communication channels with staff to address assisted living scheduling concerns, preferences, and requests promptly. Encourage collaboration among team members to cover open shifts, swap shifts, or find coverage when needed. This fosters a supportive work environment and ensures that staffing needs are met with adequate coverage.
5. Continuously Monitor and Evaluate Scheduling Effectiveness
Regularly assess the effectiveness of your staff scheduling practices by tracking key performance indicators, such as overtime rates, staff turnover, and resident satisfaction. Use this data to identify areas for improvement and implement necessary changes to enhance staff scheduling efficiency and overall facility operations.
How to Level-up Your Scheduling With Assisted Living Scheduling Software
One residence director was able to reduce expenses and improve efficiency by implementing automated scheduling software, which slashed the amount of time spent on staff scheduling each week from 20 hours to 5 hours:
Before Using Scheduling Software
- 20 hours a week spent on staff scheduling
- Difficulties communicating schedules
- Difficulties following union rules on seniority
- Difficulties recording absences
After Using Scheduling Software
- 5 hours a week spent on staff scheduling
- Internal employee communication platform & online access to schedules for staff
- Easy compliance with regulatory and union requirements by sorting employees by seniority and maintaining transparent records of actions
- Automated timesheet management
Conclusion
Nursing homes and long-term care facilities aiming for a five star quality rating need to go the extra mile in all areas of operations. This includes having qualified personnel, respecting government regulations, and promoting recently enhanced amenities to demonstrate consistently better quality care for residents.
By providing training to ensure staff have the required skills, balancing skills sets to deliver quality care, and using a workforce management tool to improve key decision-making criteria for staffing in their nursing homes, frontline managers can eliminate the many complex problems they face with staff scheduling—one of the biggest hurdles to staying at the top of the star quality rating system.
Don’t let the chronic labor shortage hold your assisted living facility back. With Agendrix scheduling software, you can optimize your staffing management, streamline your shift schedules, and boost staff morale.
- Improved staff satisfaction and retention through flexible scheduling options.
- Reduced overtime costs and better workload distribution, leading to lower labor costs.
- Enhanced communication and collaboration among team members.
- Real-time updates and notifications for schedule changes.
Try Agendrix scheduling software today and see the difference it can make in your staffing management.
What Does a Scheduler Do in a Nursing Home?
A scheduler in a nursing home is responsible for creating, managing, and updating employee work schedules to ensure adequate staffing levels for delivering quality care to the residents.
Key tasks include:
- Coordinating employee availability, time-off requests and shift preferences.
- Ensuring compliance with regulations and policies.
- Monitoring and adjusting schedules based on staffing needs.
- Managing last-minute changes due to employee absences or emergencies.
- Maintaining open communication with staff members to address concerns and resolve conflicts.
Although technology and scheduling software can aid in this process, the scheduler’s role still requires a strong understanding of the facility’s culture and the ability to build effective working relationships with the staff.
How Do I Create a Nursing Home Schedule?
- Assess staffing needs: Evaluate the nursing home’s current resident population, their care requirements, and the necessary staff-to-resident ratio to provide optimal care. Consider factors like resident acuity, required certifications, and skill levels needed for various tasks. Some tasks must be done by skilled staff.
- Gather employee availability: Collect information about each employee’s availability, preferences, and time-off requests. Consider factors like part-time and full-time status, overtime policies, and any legal requirements regarding working hours and breaks.
- Focus on staffing shifts based on seniority and skills: Distribute shifts among staff members, taking into account their seniority, skills, and expertise. Ensure that each shift is staffed with the right mix of employees to meet the residents’ needs effectively.
- Ensure compliance with regulations and policies: While creating the schedule, make sure to comply with labor laws, union agreements, and any facility-specific policies, such as minimum staffing levels, overtime restrictions, and mandatory breaks.
- Communicate and adjust the schedule: Share the finalized schedule with all staff members, allowing ample time for them to review and plan their personal lives accordingly. Be prepared to make adjustments as needed in response to last-minute changes, staff absences, or emergencies, and maintain open communication with employees to address any concerns or conflicts.